28 April, 2026
Hot Off The Press
World Research Summary
by Dr Catherine Civil.
I found some more fun and interesting articles this month to tickle your interest.
Read on …..
Next generation bionic eyes which use retinal implants
Current retinal implants can be bulky and complex, and need high-intensity visible light to work, which can damage the fragile photoreceptor cells. This new system uses nanotechnology to avoid the bulkiness and uses near-infrared light instead of high intensity visible light, which doesn’t damage the photoreceptors. Win-win.
The camera glasses connect to the ultrathin new system implanted on the retina, via Bluetooth, so there are no external cables or electronics. Then from the retina, the visual impulses travel as per normal, via the healthy optic nerve to the visual cortex where the brain “sees”.
So far, this system has only been tried on rat retina models, so it will be a while before we see it in human use, but this is a great stride forward. It is currently being promoted for macular degeneration and RP, but I don’t see why it couldn’t work for most IRDs as long as the optic nerve is intact.
Next generation bionic eyes which bypass the retina
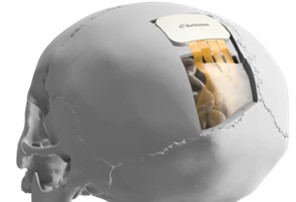 (Image credit: ReVision Implant)
(Image credit: ReVision Implant)
This is another new type of bionic eye.
This “ReVision” implant is having the first human trial this year, and a bigger trial planned over 6 months next year. The development is being fast tracked in the USA.
The wearer puts on camera glasses which transmit electronic signals directly to the brain, bypassing the eyeball in the same way that a cochlear implant bypasses the ear.
The visual impulses generated by the glasses are transmitted via a thin cable, and then a connector attached to the scalp, to hundreds of ultra-thin and durable flexible wires, which are secured on the brain surface, and implanted individually into different parts of the visual cortex at the back of the brain.
The wearer does not see in the way that we do but learns to recognise electrical patterns. The wearer should be able to navigate environments, detect obstacles such as cars and pedestrians, recognize objects, and possibly even recognize faces, with the “vision” improving with time and use.
It sounds like a big step forward in bionic eyes….. Very exciting……!
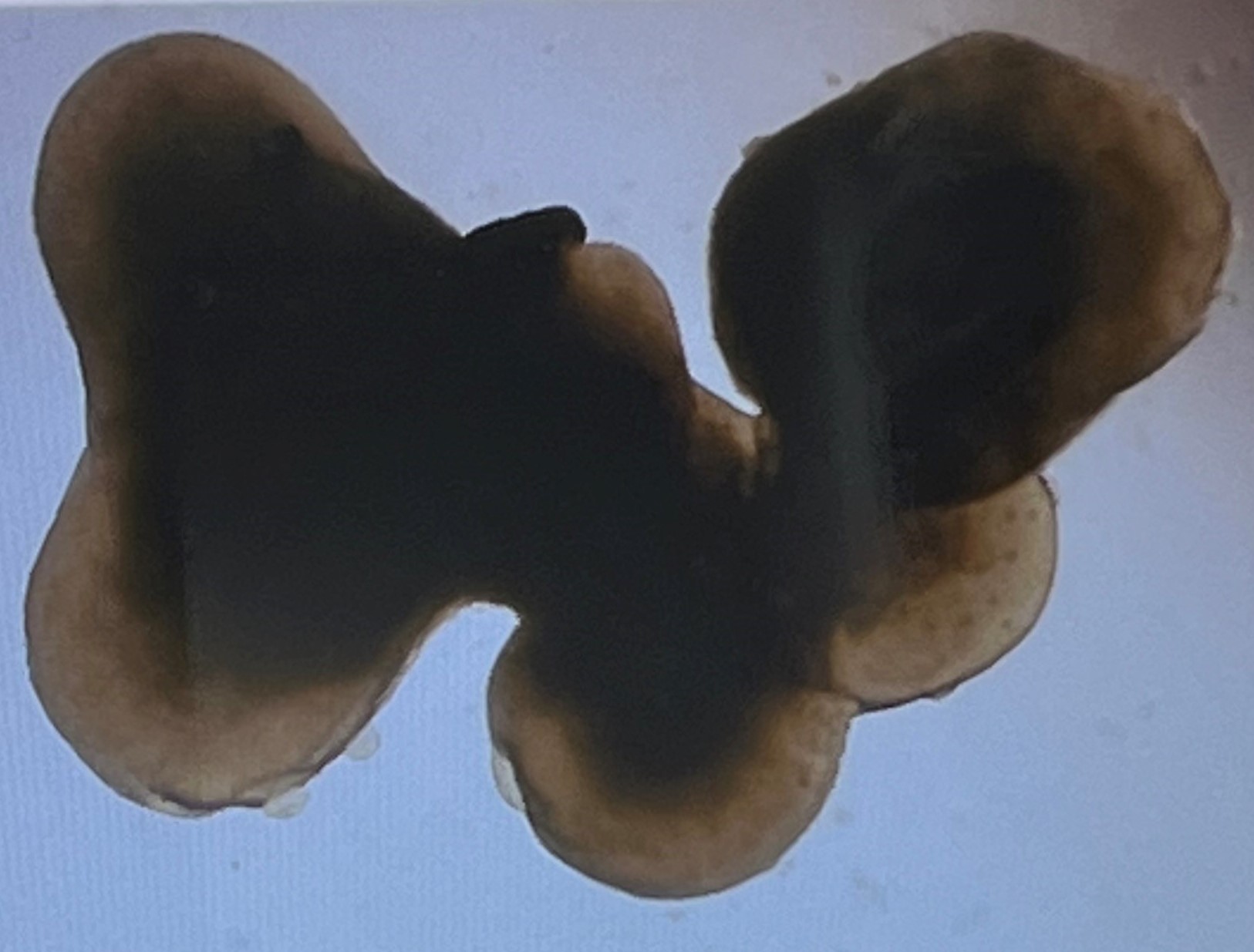
Retinal organoid study identifies pathways and compounds to protect cone cells
Cone photoreceptors are concentrated in the macula, and are essential for reading, recognizing faces, and seeing colours.
Losing them leads to the loss of central vision as we see in macular degeneration in particular. Despite many years of research, no useful treatments have been found which can stop this central damage.
However, new technology using lab grown retinal organoids means that thousands of different compounds can be tested for their positive and negative effects on the retina in a relatively short time. In this study, several useful molecules were found, and the researchers believe a “casein kinase 1 inhibitor” in particular, could be a very useful treatment in the future.
Trials for Dry AMD related Geographic Atrophy
It makes a change to see trials for dry AMD treatment as opposed to wet AMD. There are a couple of early stage 1/2 trials below for one-off intravitreal therapies for which you can check out:
Trials for Wet AMD
These trials are designed to reduce the number of treatments necessary for wet AMD. There are a few going on.
Gene therapies designed to provide long-term anti-VEGF from a single procedure including 4D-150 (Phase 3), Ixo-vec (Phase 3) and RGX-314 (Phase 3).
Long-acting drugs, such as Eylea HD and Vabysmo, and implants that slowly release medication over months, such as Susvimo.
New drug classes such as tyrosine kinase inhibitors (TKIs) including EYP-1901 (Phase 3) and OTX-TKI (Phase 3).
These strategies all aim for the same outcome: fewer injections, fewer appointments, and less disruption to daily life. Great!
That’s all folks!
Till next time …
Cathy
Guest writer – Dr Catherine Civil
My name is Dr Catherine Civil. I have been associated with Retina Australia since the early 2000s. At that time, they were called WARPF, or the WA Retinitis Pigmentosa Foundation. WARPF were raffling a car in a shopping centre, and it caught my eye because my dad and my uncle both had Retinitis Pigmentosa. Being a doctor and a parent, I had a particular interest and awareness, not just of the disease, but of the fact that there was a significant risk that I or my children or my relatives might have inherited it.
I turned up at an AGM and found myself on the Board and engaged in fundraising. I spent several years on the Board and met some wonderful people, and I was even Chairman for a couple of years. When I left, I started writing the “Hot off the Press” research update column for the newsletter.
I arrived from the UK in the early 1990s with my husband and twin baby girls to live in Perth for a year for a bit of sunshine and fun, and we find ourselves still having fun in WA 30 years later, and with a grown son as well.